Did you know that nearly 40% of patients with chronic skin conditions receive an incorrect initial diagnosis?

As a dermatologist, I witness this scenario unfold weekly in my practice: patients who have spent months or even years treating the wrong condition, growing increasingly frustrated as their symptoms persist or worsen.
Today, I want to share the real stories behind these mix-ups and give you the tools to advocate for accurate diagnosis and effective treatment. Whether you’re dealing with mysterious skin patches yourself or supporting a loved one through their skin condition, this guide will help you navigate the often-confusing world of chronic skin conditions.
Let me tell you about Maya, a 28-year-old teacher who came to my clinic after two years of failed eczema treatments. Her previous doctor had prescribed steroid creams and moisturisers, but the thick, scaly patches on her elbows and knees kept returning. Within minutes of examining her skin, I could see the telltale signs of plaque psoriasis: well-defined, raised lesions with silvery scales that her previous treatments had actually been making worse.
Then there’s Amit, a 35-year-old man with wheatish skin, whose psoriasis went undiagnosed for three years because the condition appeared as dark purple patches rather than the “textbook” red lesions most medical resources depict. His case highlights a critical issue in dermatology: conditions often present differently on darker skin tones, leading to delayed or incorrect diagnoses.
These stories aren’t unique. They represent a systemic challenge in skin condition diagnosis that affects millions of patients worldwide.
I will help you differentiate between eczema and psoriasis based on its location, the itching you experience, triggers and patterns, and associated connections. At the end of this blog, you will find a quiz to judge your situation.
Before we begin differentiating, here’s what both conditions mean:
Psoriasis is an autoimmune condition in which the immune system causes skin cells to multiply too rapidly. This creates thick, scaly, silvery patches (plaques) that are often raised and well-defined. It’s chronic and non-contagious and tends to appear on elbows, knees, scalp, and lower back. The patches are typically dry and may crack or bleed.
Eczema (atopic dermatitis) is an inflammatory skin condition that causes red, itchy, inflamed patches. The skin appears rough, leathery, or weepy, and the affected areas are usually less well-defined than psoriasis plaques. It commonly affects the face, hands, inner elbows, and the back of the knees. Eczema is often triggered by allergens, irritants, or stress, and tends to run in families with a history of allergies or asthma.
Key Difference: Psoriasis creates thick, scaly plaques due to rapid cell turnover, while eczema causes inflamed, itchy patches due to skin barrier dysfunction and inflammation.
With that being said, now let’s dive deep.
One of the most reliable ways to distinguish between psoriasis and eczema is to understand where each condition typically appears on the body. Think of your skin as a map, with each condition having its preferred territories.
This isn’t a hard rule; both conditions can appear anywhere, but location patterns provide valuable diagnostic clues.
I often tell patients to photograph their affected areas over time, noting which locations flare up most frequently.
The way your skin looks and feels can tell a compelling diagnostic story. Here’s what I look for during examinations:
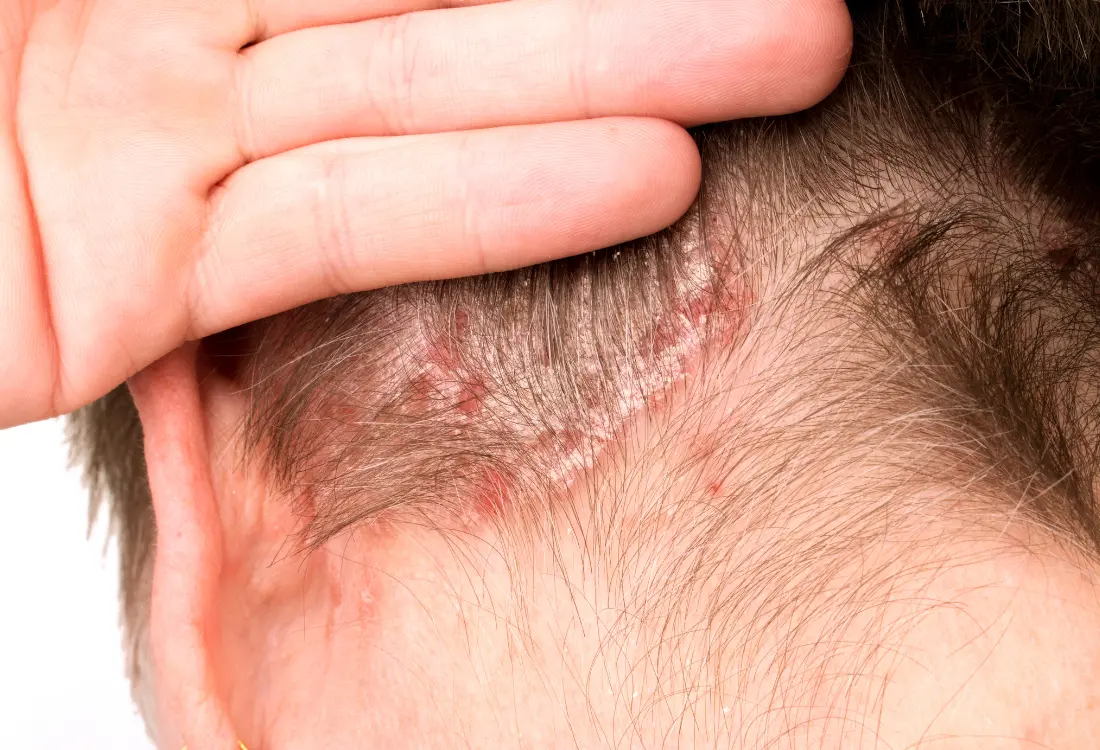
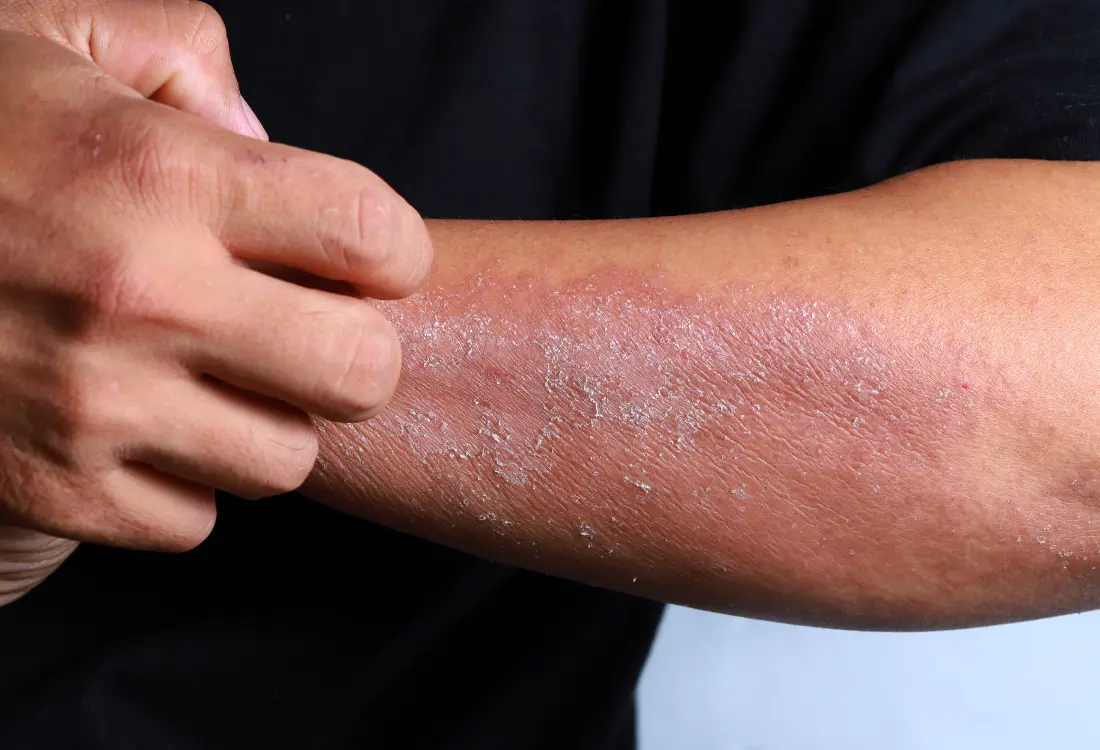
The intensity and quality of itching can provide crucial diagnostic information. Patients consistently describe these differences:
One patient described her eczema itch as “feeling like fire ants crawling under my skin,” while patients with psoriasis more commonly report “tightness and occasional irritation.”
Understanding when and how your symptoms began can provide valuable diagnostic clues:
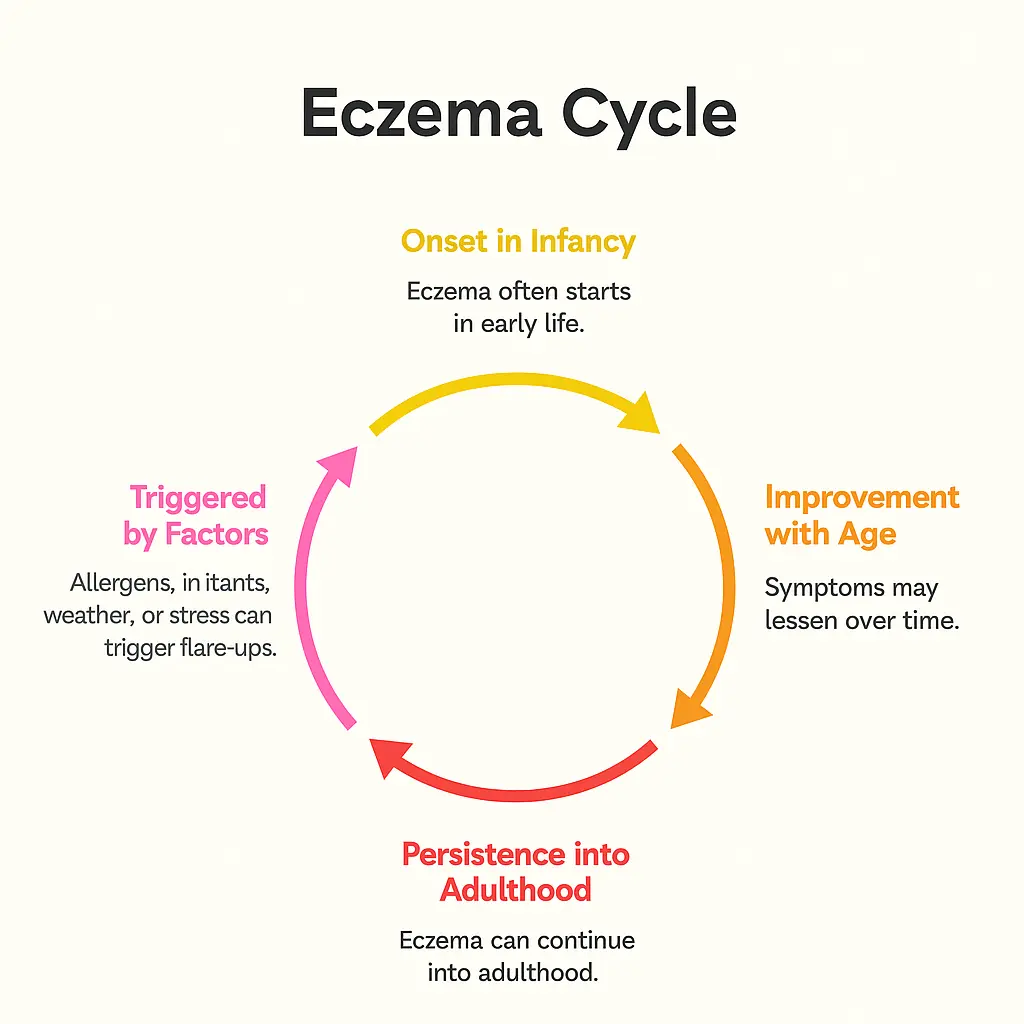
Both conditions affect more than just your skin, but in different ways:
Understanding these connections helps explain why proper diagnosis matters beyond just skin comfort.
Important Note This assessment is designed to help you understand when professional evaluation is needed, not to replace medical diagnosis. Only a qualified dermatologist can accurately diagnose skin conditions. |

Check any that apply to your situation:
If you checked ANY of these boxes, contact a dermatologist or urgent care immediately.
Check any that apply:
If you checked 2 or more boxes, schedule a dermatology consultation.
Check if any apply:
If you checked ANY of these, seeking a second opinion is reasonable and appropriate.
The treatments for psoriasis and eczema are fundamentally different because the underlying disease processes are different:
Using the wrong treatment approach can actually make some conditions worse. I’ve seen patients whose psoriasis flared dramatically when treated with eczema protocols, and vice versa.
Regardless of your specific diagnosis, some principles apply to managing any chronic skin condition:
Both conditions can significantly impact mental health. If your skin condition affects your emotional well-being, don’t hesitate to seek counselling or support groups. Many patients find that addressing the psychological aspects of chronic skin conditions improves their overall treatment outcomes.
If you’re reading this because you’re struggling with undiagnosed or poorly controlled skin symptoms, know that effective treatments exist for both psoriasis and eczema. The key is getting an accurate diagnosis from a qualified dermatologist who takes time to understand your unique presentation.
When it comes to your skin, you are your own best advocate. If your current treatment isn’t working or your diagnosis doesn’t seem to fit your experience, it’s completely appropriate to seek a second opinion. Your skin health is worth the investment in proper diagnosis and treatment.
If you’re struggling with chronic skin symptoms, our dermatology practice offers comprehensive evaluations and personalised treatment plans. Contact us.
Medical Disclaimer: This information is for educational purposes only and should not replace professional medical advice. Always consult with a qualified healthcare provider for accurate diagnosis and treatment recommendations.
The names of patients are hypothetical and do not bear any resemblance to actual individuals.